Related Topics
Do you seem to get a full night’s sleep—but then wake up feeling tired and groggy? Have you been told you snore loudly? You could have sleep apnea, a disorder that causes a person to repeatedly stop breathing while they sleep.
The most common type of sleep apnea is called obstructive sleep apnea, which happens when muscles in the back of the throat relax during sleep. This blocks up the airway, reducing or stopping airflow into the lungs. When you stop breathing, your brain alerts you to take a breath. However, this wake-sleep pattern is disruptive to deep, restorative slumber.
If you think you have sleep apnea, it’s important to make an appointment with your primary care provider or a sleep specialist as soon as possible. This condition not only causes daytime sleepiness; it can lead to serious and often life-threatening complications like heart failure, liver problems, and type 2 diabetes. Fortunately, treatments are available to address sleep apnea and help you get the restful sleep you need.
What is obstructive sleep apnea and how does it impact older adults?
Roughly 6 million Americans have been diagnosed with sleep apnea. But in reality, this sleep disorder is thought to affect 30 million people in the U.S.1 Older adults are much more likely to have sleep apnea than younger people. One study found that 56% of people age 65 and older have a high risk of developing obstructive sleep apnea.2
While sleep apnea is more common in men before the age of 50, it occurs at about the same rate in men and women after age 50.
Obstructive sleep apnea symptoms
What are the warning signs of obstructive sleep apnea in older adults? There are many, and include:
- Feeling tired and unrested when you wake up in the morning
- Headaches and/or a dry mouth when you first wake up
- Excessive daytime fatigue and grogginess
- Napping or falling asleep during the day
- Inability to focus and/or memory issues
- Snoring (often at high volume)
- Irritability, anxiety, and depression
- Sexual dysfunction
Another symptom of sleep apnea is visible pauses in breathing. If you sleep alone, you might not realize it’s happening. But if you have a partner, they may notice disruptions in your breathing at night (such as gasping for air or loud snoring interrupted by moments of silence).
How do you confirm a sleep apnea diagnosis?
To confirm a diagnosis of sleep apnea, your health care provider will likely review your medical history and ask you questions about your sleep routine and symptoms. They may want to perform a physical exam as well. If your provider suspects obstructive sleep apnea, the next step is usually a test called a polysomnogram, also known as a sleep study.
A sleep study is usually done overnight at a hospital or special sleep center (“sleep lab”). You’ll be made comfortable in a bed and hooked up to painless sensors that track your breathing, heart rate, blood oxygen levels, and brain waves to detect any unusual patterns.
If you prefer the familiarity of your own bed, sleep studies can also be done at home using a wearable monitor. A home-based sleep study can measure your heart rate and other vital signs, but it cannot track your brain activity like the specialized equipment in a sleep lab.
What are treatment options for obstructive sleep apnea?
Living with sleep apnea can be challenging, but there are treatment options that can help. Treatment for obstructive sleep apnea varies, depending on the severity of your condition and the underlying cause. Below are some common approaches.
Lifestyle changes
If your sleep apnea is mild, your health care provider may suggest you do the following to help promote healthy respiration:
- Lose weight, if you have excess weight or obesity
- Quit smoking, if you currently smoke
- Limit your alcohol intake, especially at night
- Sleep on your side (not your back)
- Increase your physical activity
- Use an allergy medication or a decongestant
- Consider finding the best mattress for you
Your provider may also advise you to avoid taking any sedating medications, such as sleeping pills.
If these simple changes don't improve your sleep, or if you're diagnosed with a more severe form of sleep apnea, your doctor may suggest other options.
CPAP machine
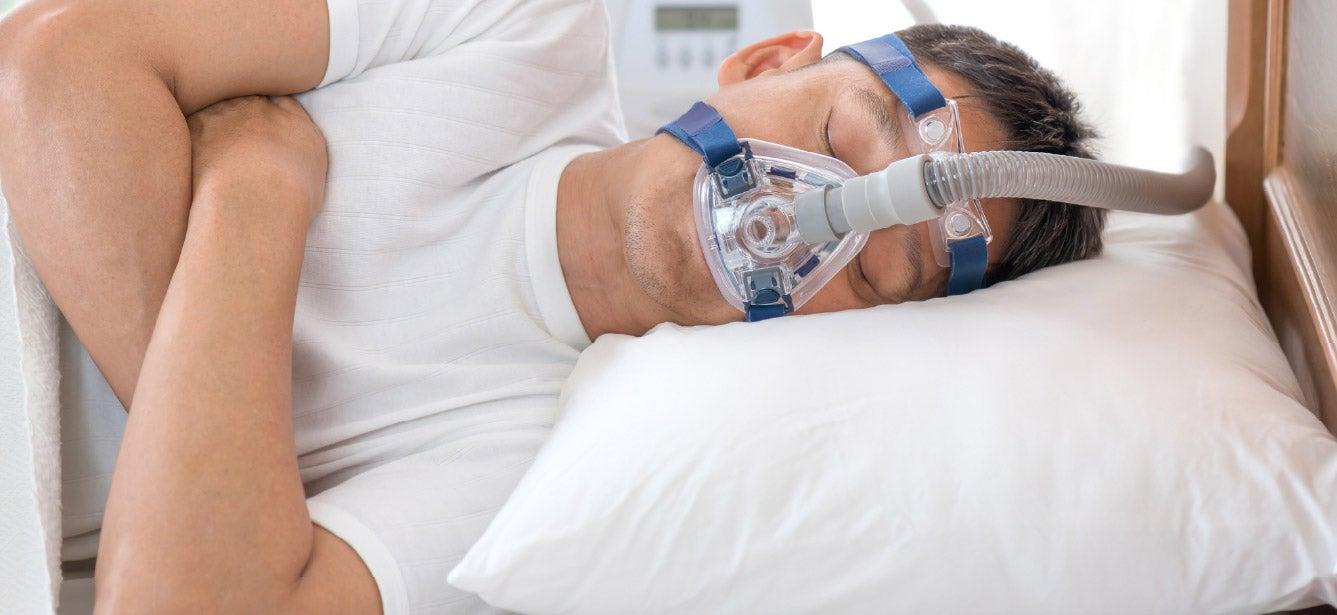
A CPAP (continuous positive airway pressure) machine involves a special mask you wear to bed at night. This mask fits into or over your nose and/or mouth and delivers constant air pressure that helps keep your airways open.
CPAP is a widely used sleep apnea treatment and considered highly effective. However, for some older adults, the mask can be uncomfortable (or too loud). The good news is the CPAP machine has evolved in recent years, and newer versions are smaller and quieter. Plus, there are many CPAP mask options available. If your doctor recommends a CPAP, be sure to try different masks to find the most comfortable fit.
Oral devices
An oral device is a custom-fit appliance you wear in your mouth during sleep. These are usually made by a dentist or orthodontist with specialized knowledge in sleep medicine appliances. Although oral devices work in different ways, their goal is the same as the CPAP machine: to keep your airways open while you’re asleep.
Surgeries of the mouth, nose, and throat can be an effective treatment for more serious cases of obstructive sleep apnea or if other approaches fail. There are different types of surgery that may be performed. The primary goal of surgery is to widen or unblock airways by:
- Reducing extra tissue that blocks airways
- Repairing abnormalities that obstruct the flow of air
- Repairing facial structure defects that impact breathing
- Removing tonsils and/or adenoids
A new sleep apnea treatment called upper airway stimulation therapy was recently approved by the U.S. Food and Drug Administration (FDA). It involves placing a small device in the upper part of the chest during an outpatient surgical procedure. This device tracks breathing patterns and, through gentle electrical impulses, helps keep airways open during sleep.
Obstructive sleep apnea causes and risk factors
What causes obstructive sleep apnea? While this disorder can affect anyone at any age, there are certain factors that increase your risk. These include:
- Age: Sleep apnea is more common in older adults.
- Family history: If you have relatives with sleep apnea, you may be more likely to develop this condition.
- Certain medical conditions: High blood pressure, type 2 diabetes, chronic lung disease, thyroid disorders, and congestive heart failure could increase the risk of developing obstructive sleep apnea.
- Smoking: People who smoke are significantly more likely to have obstructive sleep apnea than those who have never picked up the habit.
- Obesity: Excess weight or obesity can increase the risk of obstructive sleep apnea in older adults, since extra fat around the airway can cause difficulty breathing.
- Thick neck: In some people, a larger neck circumference is associated with a smaller airway.
- Nasal congestion: Whether it's seasonal allergies or a facial structure defect, those with congested nasal passages are more likely to have obstructive sleep apnea.
Bottom line
After treatment for obstructive sleep apnea, you may start sleeping better right away—or it could take a few weeks to see results. Ask your provider about a realistic timeline for recovery.
The biggest factor in treatment success is typically consistency. Sticking to your obstructive sleep apnea treatment guidelines will help ensure a better outcome. If you’re struggling to follow your treatment plan for any reason, mention it to your doctor right away.
Frequently asked questions
Can obstructive sleep apnea be treated?
Yes. Treatment for obstructive sleep apnea may include lifestyle changes, using a CPAP machine, and wearing oral devices that help keep airways open during sleep. In more severe cases, surgery can help address physical problems that disrupt the flow of air to the lungs.
What is the most common treatment for sleep apnea?
The most common treatment for sleep apnea is a CPAP machine. This treatment option involves the use of a mask that fits over a person's nose and/or mouth. Worn during sleep, the CPAP delivers steady air pressure to keep the airways open.
How do you treat obstructive sleep apnea without CPAP?
Although CPAP is considered an effective treatment for sleep apnea in older adults, it may not be right for everyone. More conservative treatments for obstructive sleep apnea may include losing weight, using a mattress for side sleepers or a mattress for sleep apnea, quitting smoking, and exercising more. In addition, a custom-fitted oral appliance worn at night can help open the upper airway by repositioning the jaw or tongue.
Sources
1. American Medical Association (AMA). What doctors wish patients knew about sleep apnea. April 1, 2022. Found on the internet at https://www.ama-assn.org/delivering-care/public-health/what-doctors-wish-patients-knew-about-sleep-apnea
2. American Academy of Sleep Medicine. Study Finds High Rate of Undiagnosed Sleep Apnea in Older Adults. May 11, 2018. Found on the internet at https://foundation.aasm.org/aasm-foundation-study-published-jags/


