Related Topics
Barbara Grassley, wife of Sen. Chuck Grassley of Iowa, is a longtime breast cancer survivor and screening advocate. She first learned of her cancer in 1987 when she noticed a large lump in one of her breasts and went to see her doctor to get it checked. Soon after, Grassley found out it was breast cancer.
She received a radical mastectomy in one breast and a lumpectomy in the other and has been cancer-free since. Grassley is now a fierce advocate for breast cancer prevention and early detection, working with the Prevent Cancer Foundation to spread the word about screening.
Mrs. Grassley encourages everyone to get their routine cancer screenings scheduled and make sure their family, friends and neighbors are aware of the importance of screening as well.
“Well, you know, it never hurts to encourage your neighbor either. Say to them you’re having your check up and ask, ‘When is yours?’” Mrs. Grassley said. “Just a little nudge here and there… Just keep on getting checked!”
Why are breast cancer screenings important for women?
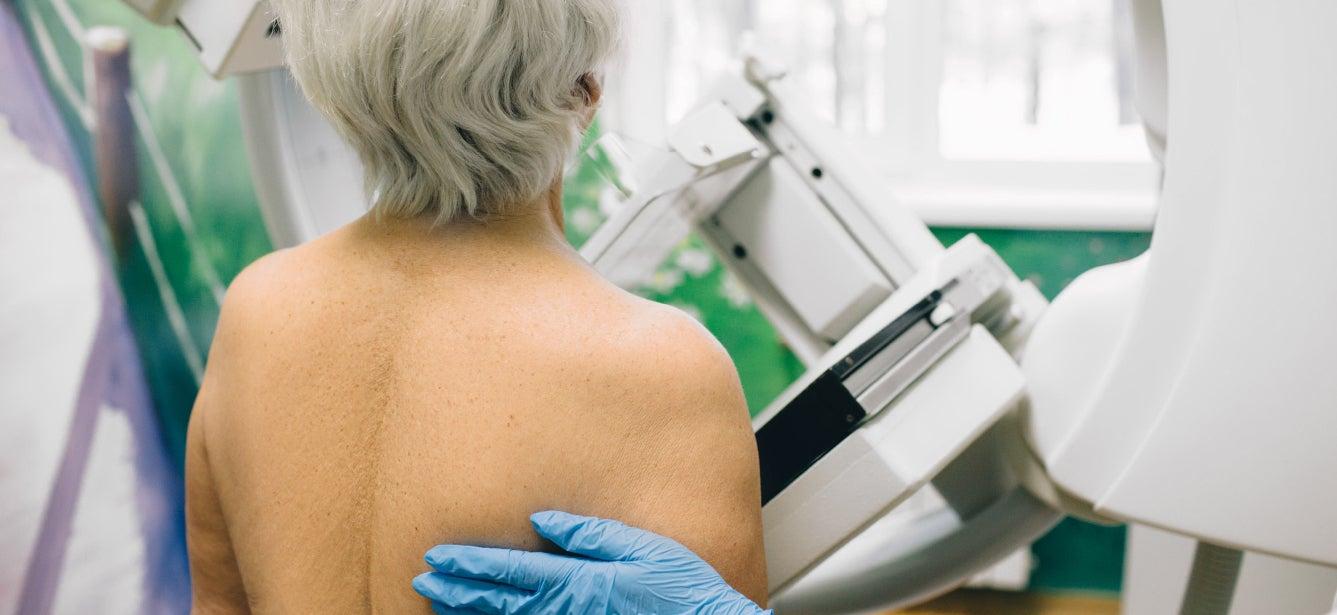
Here is the good news: breast cancer is highly treatable if found in the early stages when treatment is more likely to be successful. According to the Centers for Disease Control and Prevention, most breast cancers are diagnosed after age 50.1 Mammograms are an important and effective tool for the early detection of breast cancer. Yet, the Prevent Cancer Foundation's 2024 Early Detection survey found that 1 in 3 women ages 40 or older say they are not up to date on their breast cancer screenings.
When should I start screening for breast cancer?
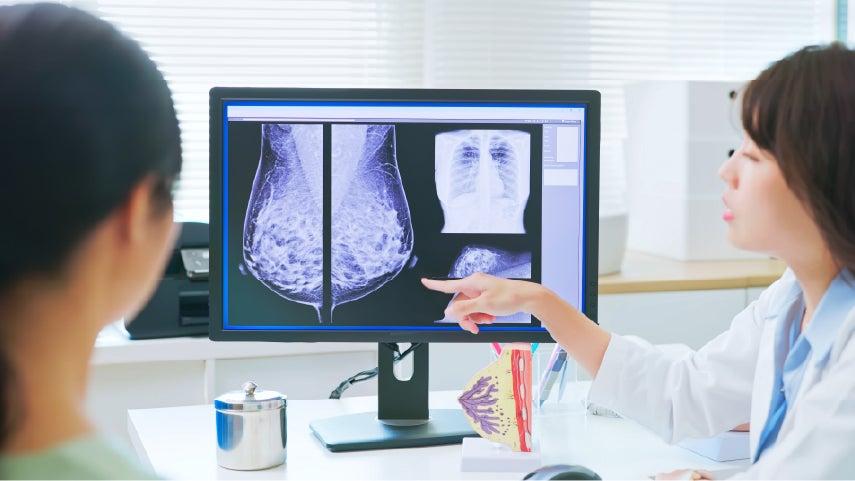
At age 40, you should begin annual screening with either traditional film (2D) mammograms or breast tomosynthesis (3D) mammograms. A 2D mammogram takes a photo from above and from the side of the breasts, while a 3D mammogram takes photos from a variety of angles to create a 3D image. A 3D mammogram may be more accurate and better for some people, such as those with dense breasts; talk to your health care provider about which option is best for you. If you are transgender, talk to your provider about what screenings are recommended for you.
If you have several close relatives with the disease or your mother was diagnosed with breast cancer before age 50, you may be at increased risk. Talk with your health care provider about getting screened earlier or having additional tests. Once you begin menopause, be sure to ask your health care provider about how hormone replacement therapy can affect your risk.
You may also be at an increased risk of breast cancer if your menstrual periods began before age 12 or you entered menopause after age 55, are overweight or obese, have never had children or had your first child after age 30, have a family history of colorectal or ovarian cancer, or have certain genetic mutations.
If you’re at increased risk for breast cancer, you may benefit from different screening tools, including breast magnetic resonance imaging (MRI). Your health care provider may also recommend genetic counseling and testing to better assess your risk and screening recommendations.
As of September 10, 2024, the Food and Drug Administration now requires all mammography facilities to include a breast density assessment as part of a patient’s medical report. All summaries sent to patients following their mammogram will be required to say whether their breasts are “dense” or “not dense." In addition to increasing overall breast cancer risk, dense breast tissue can make it harder for the radiologist reading the mammogram to see breast cancer. Depending on a person’s breast density and personal risk of breast cancer, next steps may include supplemental breast MRI or breast ultrasound, to help confirm the mammogram reading. Unfortunately, follow-up imaging may not be covered by insurance—posing a significant barrier to those who need it.
What are the symptoms of breast cancer?
While routine screenings are important in finding breast cancer before any signs or symptoms occur, you should also talk with your health care provider right away if you notice any of these symptoms in your breasts (regardless of when your last screening appointment was):
- A lump, hard knot or thickening in the breast
- A lump under your arm
- A change in the size or shape of your breast
- Nipple pain, tenderness or discharge, including bleeding
- Itchiness, scales, soreness or rash on your nipple
- A nipple turning inward or inverted
- A change in skin color or texture such as dimpling, puckering or redness
- A breast that feels warm or swollen
How can I reduce my risk of breast cancer?
You can reduce your risk of developing breast cancer through these lifestyle related behaviors and actions:
- Ditch tobacco. Do not smoke or use tobacco in any way. If you do, quit. (Call 1-800-QUIT-NOW for help.) Exercise for at least 30 minutes, at least 5 days a week. Make it a priority to move more and sit less.
- Consider breastfeeding (chestfeeding). Breastfeeding (chest feeding) may lower the risk of breast cancer.
- Limit your alcohol intake. If you drink, limit your drinking to no more than one drink a day if you are a woman or two a day if you are a man. Drinking alcohol is linked to breast and several other types of cancer. The more you drink, the greater your risk of cancer. Even drinking small amounts might increase your risk.
- Maintain a healthy weight. Being overweight or obese, particularly after menopause, can increase your risk of breast cancer. Exercise for at least 30 minutes, at least 5 days a week. Make it a priority to move more and sit less.
- Stay on top of your screenings. In addition to risk reduction, the most important thing one can do is to stay on schedule with breast cancer screenings and encourage friends and family to do so as well.
As Grassley encourages, “Just keep on getting checked!”
To learn more about breast cancer prevention and screening information, visit preventcancer.org/breast.
Sources
1. Centers for Disease Control and Prevention. Breast Cancer Risk Factors. Found on the internet at https://www.cdc.gov/breast-cancer/risk-factors/index.html#:~:text=Most%20breast%20cancers%20are%20found,factors%20have%20the%20same%20effect